The article below featuring Lighthouse Biomedical was originally futured in the Brightlands Maastricht Health Campus Glossy about 2021. Download the full glossy. Learn more about their work at Medace here.
Aart van Apeldoorn is an assistant professor at MERLN, where he is working on a new stem cell therapy for type 1 diabetes. Aart developed an innovative implant for cells that produce insulin. His partner Vanessa LaPointe is bringing his invention to market through the new company Lighthouse Biomedical.
“Thanks to this small sheet of cultivated cells, diabetes patients will no longer need to inject insulin in the future”
It is impossible to pinpoint a real eureka moment. The process consisted of many isolated moments,
each taking the invention a step further over the years. If there was a decisive moment, it was a phone call from Leiden. ‘As a bioengineer at the University of Twente, I had been working on a study of bone and cartilage about fifteen years ago. However, I wasn’t sure whether I wanted to continue doing it. At the right moment, I received a phone call from Professor Eelco de Koning, who was researching Type 1 diabetes in Leiden. He was looking for an alternative to the existing treatment with the islets of Langerhans. These groups of cells are transplanted from a donor pancreas to the liver of a diabetic patient, where they produce insulin so that the patient no longer needs to inject it.’
‘That established therapy has a couple of major drawbacks: to prevent the cells from being rejected immediately, you have to shut down the patient’s entire immune system. And even then, 60-70% of the cells are broken down. Eelco asked me to take on a bioengineering approach to contribute to a more efficient treatment method. That really appealed to me. Internationally, hardly anyone in our field was researching this at the time, so if we could do it, we would really make a difference.’
‘The goal was to make a medical device with cultured cells that bypass the immune system and therefore have a greater chance of survival. Our preference was for an open structure in which all cells get enough oxygen rather than a closed implant, where all cells are clumped together. What we have ultimately developed is a kind of sheet with a special structure in it, made of a biomaterial. In it, we can capture and hold small spheres of cells that produce insulin.’
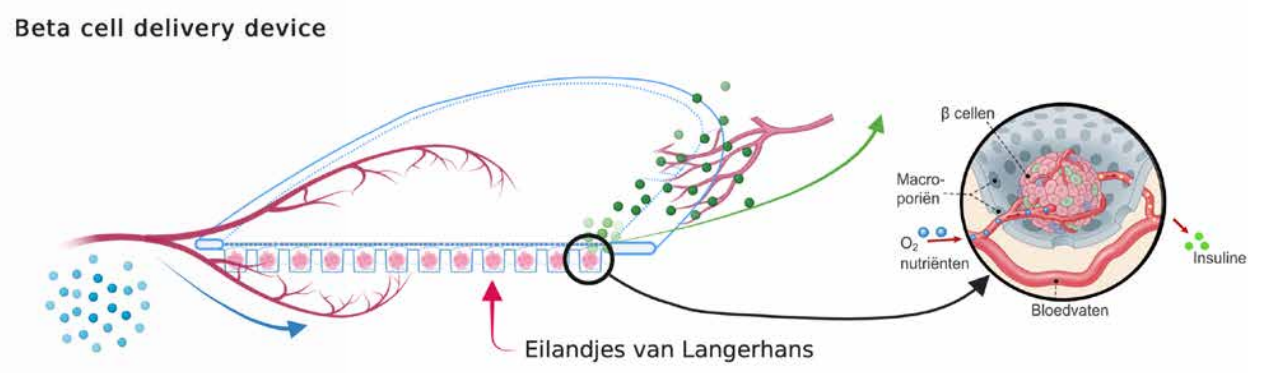
‘A large part of our research consisted of choosing the right biomaterial. We grew beta cells on all kinds of materials and discovered on which material the stress in the cell is lowest. You could call that a eureka moment.
Ultimately, the device will be implanted in an area of the body that has lots of oxygen-rich blood. This would be outside the liver, where the cells are more likely to survive. The search for that ideal spot also provided another eureka moment.’
‘For such research, you need to be in it for the long haul. Ten years can just fly by. Over the last four
years, we have been able to make great strides at MERLN. The fact that we are part of the RegMed XB consortium has certainly helped. We are hopeful that the clinical trial can start at the end of 2022. Only in about seven years’ time will we know whether this new method of treatment has really helped patients.’
‘In recent years, I have regularly explained this research during evening meetings scheduled for patients. The enthusiasm and commitment of this group of patients provides much motivation to continue. I think it’s fantastic that the prospect that our invention can dramatically improve the quality of life of these people.’ Lighthouse Biomedical
